In years 1-3 of the iTech, we will have optimized and pilot-tested using a similar study design and identical study outcomes two distinct mobile apps, LYNX and MyChoices, designed to increase HIV testing and PrEP uptake among YMSM. The apps were developed based on different theories of behavior change, and therefore contain different components, differing messaging strategies and different approaches for engaging youth. If either or both apps are shown to be both feasible and acceptable, the individual apps will be tested in this follow-on research study in Years 4 and 5 to evaluate for efficacy. Comparing the apps will allow us to identify any efficacy differences in increasing HIV testing or increasing PrEP uptake between the two apps. If justified, we will combine the components of each app that have the greatest impact on behaviors into a final, composite app for dissemination.
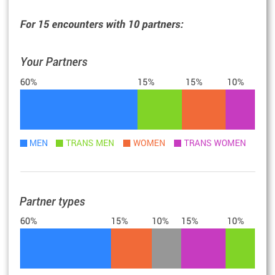
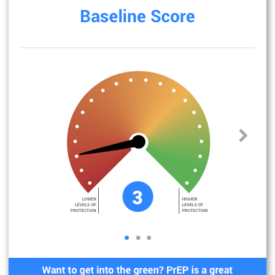
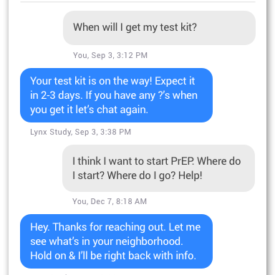
Screenshots
Duration
Intervention lasts 12 months.
Sample Size
Approximately 450 YMSM in 7 iTech SRVs (~56 per site) will be enrolled and randomized (1:1:1) to one of three conditions: 1) the MyChoices app and provision of referrals to local HIV/STI testing and PrEP resources (n=154); 2) the “LYNX” app and provision of referrals to local HIV/STI testing and PrEP resources (n=154); or 3) standard of care provision of referrals to local HIV/STI testing and PrEP resources (i.e., SOC) (n=154). Randomization will be stratified by site and age (15-18, 19-24).
Eligibility
- Age 15 to 24 years.
- Assigned male sex at birth and male identified.
- Self-report being HIV uninfected or HIV status-unknown at screening.
- Owns or leases a phone with Android platform or iOS platform, has an active data plan
- Willing and able to attend an in-person baseline study visit in one of the study site areas
- More information on eligibility and exclusion criteria available on ClinicalTrials.gov
Primary Outcomes
- HIV Testing
- PrEP uptake
Secondary Outcomes
- HIV/STI testing
- Self-reported STI testing
- Participants will be asked about frequency and results of all HIV/STI tests
- Participants will be asked to sign medical release forms for the release of their testing results from the respective testing site so that study staff can collect official results through medical record abstraction
- PrEP interest
- Sexual behaviors, including frequency of condomless anal sex
- IMB and SCT model constructs
- App usage patterns: To determine app usage patterns, we will use app analytics to determine whether at least 60% of individuals randomized to the intervention conditions opened the apps at least 2 time after their initial introduction to the app by research staff by the 12-month follow up assessment. We will also assess time spent on each app function.
- Time spent on each component of the intervention and costs attributed to that time will be evaluated, including but not limited to home test kits, creating databases of local testing areas, and app maintenance.